|
Key Takeaways:
|
Diabetes and cataracts are two common health issues that affect a significant portion of the population. While they may seem unrelated, there is evidence to suggest a potential link between the two conditions. This article aims to explore this potential relationship and shed light on how managing diabetes can help prevent cataracts.
Cataract is a condition characterized by the clouding of the lens in the eye, leading to blurred vision. It is commonly associated with aging, but other factors such as diabetes can also contribute to its development. Diabetes, on the other hand, is a chronic condition characterized by high blood sugar levels. It can affect various organs, including the eyes.
By understanding the potential interrelation between diabetes and cataracts, individuals can take proactive steps to protect their eye health and overall well-being. Let’s delve deeper into this topic and uncover the key insights.
How Diabetes Affects Cataract Risk
Vision is one of the most precious senses we have, yet disorders like cataract and diabetes can silently threaten it over time. While cataracts are often linked with ageing, people with diabetes are at a significantly higher risk of developing them earlier and progressing faster. In this detailed blog, we explain how cataract and diabetes are connected, the symptoms to watch out for, and why timely treatment is essential to preserve your sight.
What Are Cataracts? A Clearer Lens With a Cloudy Problem
A cataract is a condition in which the normally clear lens of the eye becomes cloudy or opaque, leading to blurred vision. Under normal circumstances, the lens enables light to pass through to the retina at the back of the eye, where images are formed. When cataracts develop, this clarity is lost, making vision misty or foggy.
Why Cataracts Form
Cataracts occur when proteins in the eye’s lens start breaking down and clumping together. This disrupts the smooth path of light entering the eye, resulting in clouded vision. While age-related cataracts are the most common, typically occurring as a part of natural ageing, several other factors can accelerate their development.
What Is Diabetes and Why It Matters for Eye Health
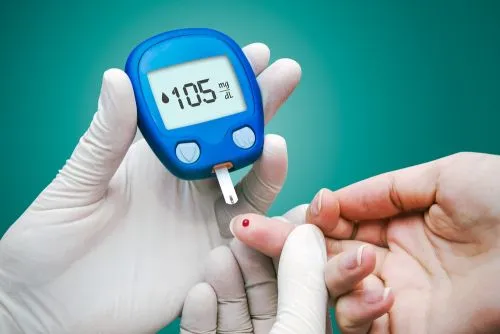
Diabetes is a chronic metabolic disorder characterised by elevated blood sugar (glucose) levels, resulting either from insufficient insulin production or the body’s inability to use insulin effectively. Over time, persistently high blood sugar can damage blood vessels and tissues throughout the body, including delicate structures in the eyes.
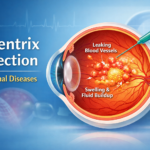
This is where the connection between diabetes and eye conditions, such as diabetic retinopathy and cataract, becomes crucial.
How Cataract and Diabetes Are Interrelated
1. High Blood Sugar Accelerates Lens Changes
People with diabetes are at a significantly greater risk of developing cataracts than those without diabetes. High blood glucose alters the normal balance of fluids and proteins within the eye lens. Enzymes convert excess glucose into sorbitol, a sugar alcohol that builds up and draws in fluid. This leads to swelling and structural changes in the lens proteins, making it cloudy over time – the hallmark of a diabetic cataract.
2. Earlier Onset and Faster Progression
Cataracts in individuals with diabetes tend to occur at a younger age and progress more rapidly than in those without the disease. In fact, studies show that cataract prevalence is markedly higher in diabetic populations, with some research suggesting that people with diabetes are up to four times more likely to develop cataracts compared to non-diabetics.
This accelerated progression may be due to ongoing oxidative stress, sorbitol accumulation, and glucose-caused changes in lens clarity – all consequences of prolonged elevated blood sugar levels.
3. Diabetes Increases the Risk of Multiple Eye Disorders
In addition to cataract, people with diabetes are also predisposed to other serious eye conditions, including diabetic retinopathy (damage to retinal blood vessels) and glaucoma (increased pressure damaging the optic nerve). These conditions can coexist with cataracts and compound the risk of vision loss if not monitored regularly.
Signs and Symptoms — Knowing What to Look For
Early detection of eye changes due to diabetes is vital. Symptoms of cataracts, including diabetic cataract, can be subtle in the beginning but worsen over time. Pay attention to the following signs:
- Blurred or cloudy vision — the most prevalent symptom.
- Increased glare and sensitivity to bright light — especially when driving at night.
- Faded or washed-out color perception — colors appear less vibrant.
- Reduced night vision — difficulty seeing in low-light conditions.
- Halos around lights — rings or circles seen around lights.
- Frequent changes in eyeglass prescription — as vision fluctuates due to swelling of the lens.
Some symptoms overlap with other eye conditions, which is why comprehensive examinations by an eye care professional are essential.
Why Timely Treatment Is Key to Preserving Vision
When left untreated, cataracts can progressively worsen to the point where daily tasks become difficult or impossible. In people with diabetes, the stakes are even higher because other diabetes-related eye complications can coexist.
The Only Effective Treatment: Cataract Surgery
Currently, no medication or eye drop can reverse cataracts. The most effective treatment option is surgical removal of the cloudy lens and replacement with a clear artificial lens (intraocular lens or IOL). Cataract surgery is one of the most commonly performed procedures worldwide and has a high success rate in restoring vision.
During surgery:
- A small incision is made in the eye.
- The cloudy lens is broken up and removed.
- A clear artificial lens is implanted in place of the natural one.
Special Considerations for People with Diabetes
If you have diabetes:
- Blood sugar control is crucial before surgery — high glucose can affect healing and increase the risk of complications.
- Co-existing conditions like diabetic retinopathy must be evaluated — even after successful cataract surgery, vision may not fully recover if the retina is damaged.
Surgery timing matters — earlier intervention can prevent the cataract from becoming too dense and causing more complex surgical requirements.
Complications — What Can Go Wrong Without Timely Care?
If cataracts are ignored:
- Vision becomes progressively impaired.
- Daily activities like reading, driving, or recognising faces become difficult.
- Increased risk of falls and accidents due to poor vision.
- Potential for blindness if combined with diabetic retinopathy or macular oedema.
Diabetes can also increase the likelihood of post-surgical complications, such as inflammation, macular swelling, or slower healing, making regular follow-up care essential.
Prevention and Eye Care Strategies for People With Diabetes
While cataracts cannot always be prevented, especially age-related ones, good diabetes management can significantly reduce risk and slow progression:
1. Control Blood Sugar and HbA1c Levels
Maintaining target glucose levels reduces the metabolic stresses that lead to lens clouding.
2. Get Comprehensive Eye Checkups
Get your eyes checked every year, even the dilated pupil part. This helps spot cataracts and other eye stuff linked to diabetes early.
3. Adopt a Healthy Lifestyle
- Eat a balanced diet rich in antioxidants (fruits and vegetables).
- Engage in regular physical activity.
- Avoid smoking and excessive alcohol.
- Protect eyes from harmful UV rays with quality sunglasses.
4. Monitor Other Health Metrics
High blood pressure and cholesterol common in people with diabetes, can increase eye disease risk, so these should also be controlled.
Conclusion — Staying Ahead of Vision Threats
The relationship between cataract and diabetes goes beyond coincidence. Elevated blood sugar levels accelerate lens changes, making people with diabetes more susceptible to earlier and more aggressive cataract formation. Diabetic cataract, while treatable, demands timely detection and intervention to prevent long-term vision loss.
FAQs
What is the link between diabetes and cataracts?
Diabetes is linked to cataracts because high blood sugar levels can cause changes in the eye lens, leading to cataract development.
Why do diabetics get cataracts?
Diabetics are more likely to get cataracts due to elevated sugar levels, causing changes in the eye lens.
What are the signs that diabetes is affecting your eyes?
Blurred vision, fluctuating eyesight, and difficulty focusing are signs that diabetes may be affecting the eyes.
Are people with diabetes more prone to developing cataracts?
Yes, individuals with diabetes are more susceptible to cataracts, often experiencing earlier onset and faster progression.
Can controlling diabetes help prevent cataracts?
Yes, managing diabetes is crucial to reduce the risk of cataracts and handle potential eye issues.
What are the treatment options for cataracts in diabetic patients?
Cataract surgery is a common and effective treatment for diabetic patients to restore vision.
Is cataract surgery safe for individuals with diabetes?
Yes, cataract surgery is generally safe for individuals with diabetes and can greatly improve vision.
Are there any precautions diabetic individuals should take before undergoing cataract surgery?
Diabetic individuals should keep their blood sugar stable and inform their surgeon about their diabetes medications.
Can cataracts in diabetic patients lead to vision loss if left untreated?
Yes, if left untreated, cataracts in diabetics can lead to gradual vision loss, stressing the importance of timely intervention.
Can diabetes increase the risk of developing cataracts?
Yes, prolonged high blood sugar accelerates lens clouding and cataract formation.
What is a diabetic cataract?
It is a cataract caused by diabetes-related blood sugar changes affecting lens clarity.
At what age do people with diabetes develop cataracts?
People with diabetes may develop cataracts earlier than non-diabetic individuals.
Can controlling diabetes prevent cataracts?
Good blood sugar control can slow cataract progression, but cannot completely prevent it.
Is cataract surgery safe for diabetic patients?
Yes, cataract surgery is safe with proper blood sugar control and monitoring.